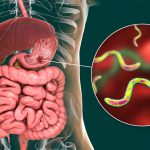
In a significant revelation, recent research suggests that gut-related problems, such as constipation, swallowing difficulties, and irritable bowel syndrome, might potentially act as early indicators of Parkinson’s disease. Published in the journal Gut, these findings bolster the notion of a close connection between brain health and gastrointestinal well-being.
Understanding the mechanisms behind gut-related concerns could potentially lead to more timely intervention and management strategies for Parkinson’s disease, according to the researchers.
Parkinson’s disease is characterized by its progressive nature, wherein the condition worsens over time due to insufficient dopamine in the brain, leading to symptoms like involuntary tremors, slow movements, and muscle stiffness.
Amid the absence of a definitive cure, available treatments aim to alleviate major symptoms and sustain a reasonable quality of life.
Detecting the disease even before neurological symptoms manifest and significant brain cell damage occurs could substantially alter its course.
The study encompassed a comprehensive analysis of US medical records, examining 24,624 individuals diagnosed with Parkinson’s, and comparing their data to those of individuals with Alzheimer’s, cerebrovascular disease, and healthy brains.
The pivotal questions the study sought to address were:
- Did patients with Parkinson’s experience gut-related issues in the six years preceding their diagnosis?
- Did individuals with gastrointestinal problems have a higher likelihood of developing Parkinson’s?
The answer to both queries was affirmative, with a duration of five years of data forming the basis.
Notably, four specific gut conditions—constipation, difficulty swallowing, gastroparesis (a delay in food movement through the small intestine), and irritable bowel syndrome—were associated with an elevated risk of Parkinson’s disease.
Interestingly, the removal of the appendix seemed to exhibit a protective effect, a correlation that has been recognized in previous research as well.
However, the researchers underline that not all individuals experiencing gastrointestinal problems will necessarily develop Parkinson’s. Nonetheless, a distinct connection between gut health and brain health appears to be evident.
The gastrointestinal tract houses numerous nerve cells that engage in communication with the brain. This presents the possibility that therapeutic interventions beneficial for one system might also yield advantages for the other, or that an ailment affecting one region could influence the other.
Parkinson’s UK representative Clare Bale underscores that these findings further strengthen the theory that gut issues might be an early warning sign of Parkinson’s disease.
Professor Kim Barrett from the University of California, Davis, notes the need for further investigations to determine whether this link could be utilized by medical professionals to aid patients.
The report refrains from attributing causality, raising the potential for an unknown third risk factor influencing both gastrointestinal conditions and Parkinson’s disease.
Nevertheless, the conclusions of this study hold clinical implications, prompting a call for additional research endeavors.
Dr. Tim Bartels from the UK Dementia Research Institute at University College London emphasizes that this study cements the gut’s potential as a prime target for the identification of Parkinson’s biomarkers—observable physical changes that could serve as early indicators.
Bartels highlights the immense value in predicting Parkinson’s disease earlier, as it could significantly enhance treatment efficacy and drug targeting strategies.